Published on:
MEDICAL MALPRACTICE, HYDROCEPHALUS
IS IT NECESSARILY MEDICAL MALPRACTICE?
By Anthony H. Gair,
Hydrocephalus is basically an overabundance of cerebro/spinal fluid within the head. Hence, the commonly used lay term, “water on the brain”. While hydrocephalus is usually thought of as occurring in the newborn it is not uncommon for adults to develop this condition.
There are a myriad of causes of hydrocephalus.
Congenital abnormalities such as Arnold-Chiari malformation, Dandy-Walker Syndrome and aqueduct stenosis among others are well known precipitators of this condition which may not manifest itself until adulthood. Acquired conditions are also known to cause a blockage in the ventricular system leading to the onset of hydrocephalus. Intraventricular hematomas, tumors, abscesses, trauma and arachnoid cysts have all been documented as precipitating hydrocephalus. Hydrocephalus has been classified as communicating (obstruction of cerebrospinal fluid flow outside of the ventricular system) and obstructive (obstruction of CSF flow within the ventricular system).
Cerebrospinal fluid is produced within the ventricles of the brain. The four ventricles of the brain, two lateral and the third and forth ventricles, are cavities or chambers within the brain. The walls of each ventricle contain a structure known as the choroid plexus which produces CSF. The CSF flows from the ventricles throughout the brain and spinal cord and is eventually absorbed through the arachnoid granulations into the venous blood of the brain. CSF is constantly produced at the rate of 0.35 ml/min or 500 ml/day. When one of the above mentioned conditions (the list is obviously not exhaustive) causes a blockage in the flow of CSF hydrocephalus results. The build up of CSF causes an increase in intracranial pressure and an expansion of the ventricles. If the CSF is not drained white matter damage, gliotic scarring, grey matter damage and death may result. The increase in intracranial pressure may also cause brain herniation.
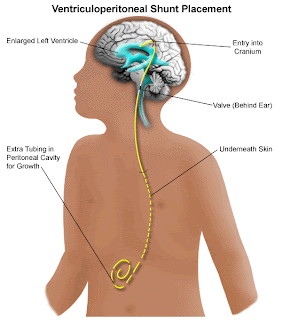
The manner in which CSF is drained in a patient, adult or child, with hydrocephalus is by means of a shunt, most commonly a ventricular peritoneal shunt. Basically, the shunt system consists of silastic tubing, catheters, a reservoir and a pressure activated valve. By means of a burr hole in the skull, a catheter is inserted into the lateral ventricle. The peritoneal catheter is inserted through the clavicular area and tunneled into the peritoneum. Under the scalp is spliced a pressure activated valve and a reservoir which allows aspiration of CSF for analysis. This, of course, is an oversimplication of the procedure, but demonstrates the way in which CSF is drained. When the intracranial pressure reaches a level at which the valve is engineered it is activated and drains the fluid thereby preventing dilation of the ventricles and a potentially lethal increase in intracranial pressure. For a detailed discussion of hydrocephalus and shunting technique, the classic multi-volume text of Dr. Julian R. Youmans, Neurological Surgery, Vol. 2, W. B. Saunders Co., 1996 edition is recommended.
Obviously, as in any foreign device, failures may take place. It is therefore incumbent upon the physician treating such a patient to be cognizant of the clinical signs of shunt failure. Debris, infection and catheter migration among others may clog the ventricular catheter. The peritoneal catheter may also become clogged or obstructed by infection, movement and other causes. Classic clinical signs of a malfunctioning shunt include severe headaches, nausea, vomiting, impaired balance, lethargy and papilloedema.
It is mandatory in a shunted patient displaying these symptoms to order a CT Scan of the brain which must be compared to a prior baseline scan and/or records of the scan, if available. An interval increase in the size of the ventricles is conclusive proof of shunt failure and necessitates surgery to revise the shunt. The situation the plaintiff’s attorney may be confronted with is where there was neither a baseline CT Scan nor records of same available to the physician for comparison. If there was such a prior CT Scan and/or records of the scan available which demonstrate an interval expansion of the ventricles and surgery to repair the shunt was not promptly performed resulting in brain damage or death of the patient, medical malpractice is usually obvious. It is, of course, not so simple when no prior CT Scan or records are available for review. What should a physician do when confronted with a patient shunted for hydrocephalus who presents, for example with intermittent severe headaches, episodes of nausea and vomiting and lethargy. A CT Scan should obviously be taken. An increase in the size of the ventricles should be viewed with suspicion. However, not all shunted patients will experience a reduction of the size of the ventricles following shunting. Therefore, a single CT Scan demonstrating an expansion of the ventricles without an available baseline scan and/or records is not conclusive evidence of shunt failure.
For many years physicians often relied on pumping the shunt (the valve) to see if there was a return of CSF to determine whether the shunt was functioning. Although shunt pumping may provide useful information, it has now been demonstrated that pumping the shunt is not an effective means of testing shunt function. Pumping the shunt will not reveal whether the valve is functioning at the pressure for which it is engineered. It will also not reveal intermittent obstruction of the shunt whether it be distal or proximal. In this regard see Youmans, supra, and Physical Examination of Patients with Cerebrospinal Fluid Shunts: Is There Useful Information in Pumping the Shunt by Piatt JH Jr. Pediatrics 1992 Mar; 89(3):470-473 and Pumping The Shunt Revisited, by Piatt JH Jr. Pediatric neurosurgery 1996 Aug. 25(2):73-76.
In a patient who presents with intermittent clinical signs of shunt failure for whom neither a baseline CT Scan nor prior records are available it may not be medical malpractice, depending on the particular case, for a physician not to immediately operate to revise the shunt. If the physician includes shunt failure as the priority in his differential diagnosis, a transfer of the patient to the intensive care unit with orders to closely observe his neurological condition, depending upon the particular case presented, may be acceptable practice. However, given demonstrated expansion of the ventricles on CT Scan, any change in the patient’s condition such as reoccurrence of headaches, vomiting or signs such as papilloedema are indication for shunt revision given that failure to do so may result in irreversible brain damage, coma and eventually death.
Reference: Image From Lucile Packard Children’s Hospital at Stanford
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog