10 Lawyers from New York Personal Injury Law Firm Gair Gair Conason Steigman Mackauf Bloom&Rubinowitz Named 2013 New York Super Lawyers

10 Lawyers from Gair Gair Conason Steigman Mackauf Bloom&Rubinowitz were recently selected by their peers as New York Super Lawyers for 2013. Our primary practice area is personal injury. We handle all types of personal injury cases including medical malpractice, car accident, product liability, construction accident and wrongful death cases. Those selected are Jeffrey B. Bloom, Seymour Boyers, Anthony H. Gair, Howard S. Hershenhorn(Top 100) ,Jerome I. Katz, Stephen H. Mackauf, Ben B. Rubinowitz(Top100), Christopher L. Sallay, Ernest R. Steigman and Richard M. Steigman.
The sum of the verdicts and settlements our attorneys have obtained approaches $1 billion dollars. We believe the key to achieving these results is to limit our case intake to approximately 80-100 cases per year so that extensive personal attention and meticulous trial preparation are afforded to each of our clients on all matters. Because we are selective in the cases we accept, we are able to immerse ourselves in our cases and as a result, we are able to resolve our clients’ cases more quickly than other plaintiff’s personal injury firms.
We operate what some might call a “boutique firm”-which means we limit our practice to a select group of serious and substantial tort cases, but our results speak for themselves. As a personal injury firm, we spend a significant amount of time deciding whether we will accept a case, and, because we only accept a select few cases, we are able to spend more resources than other firms to secure the most knowledgeable experts and to get the best results for our clients.
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog


 Accused by the Office of Professional Medical Conduct of botching surgeries,faking surgeries, performing unnecessary surgeries and prolonging the ailment of hundreds of patients, Dr. Spyros Panos, an Upstate New York surgeon formerly practicing at Mid Hudson Medical Group in Poughkeepsie, N.Y was ordered to surrender his medical license by the state Board of Professional Medical Conduct. DR. Spyro is facing over 200 medical malpractice lawsuits.
Accused by the Office of Professional Medical Conduct of botching surgeries,faking surgeries, performing unnecessary surgeries and prolonging the ailment of hundreds of patients, Dr. Spyros Panos, an Upstate New York surgeon formerly practicing at Mid Hudson Medical Group in Poughkeepsie, N.Y was ordered to surrender his medical license by the state Board of Professional Medical Conduct. DR. Spyro is facing over 200 medical malpractice lawsuits.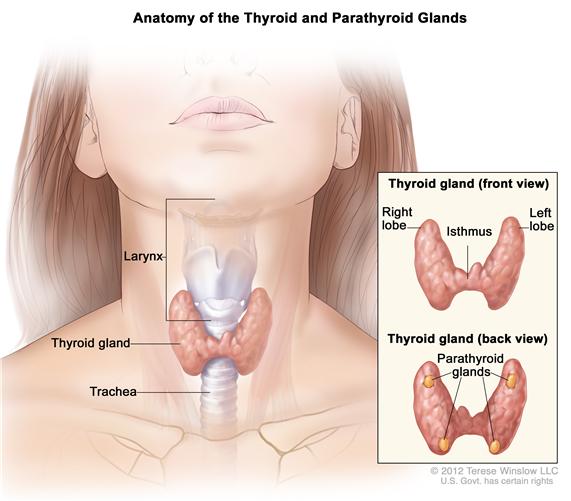 Thyroid cancer may be over diagnosed and over treated and many patients may have been exposed to unnecessary treatment and dangerous procedures according to a new study lead by Juan Pablo Brito, M.B.B.S. an endocrine fellow and health care delivery scholar at
Thyroid cancer may be over diagnosed and over treated and many patients may have been exposed to unnecessary treatment and dangerous procedures according to a new study lead by Juan Pablo Brito, M.B.B.S. an endocrine fellow and health care delivery scholar at