Proper diagnosis of Denys-Drash syndrome
Failure to timely diagnose Denys-Drash syndrome can be medical malpractice that can lead to renal failure and ultimately death. Denys-Drash syndrom is a very rare congenital disorder that affects young children. There are only 150 known cases in the world therefore very little information is available for doctors to diagnose and treat this disorder.
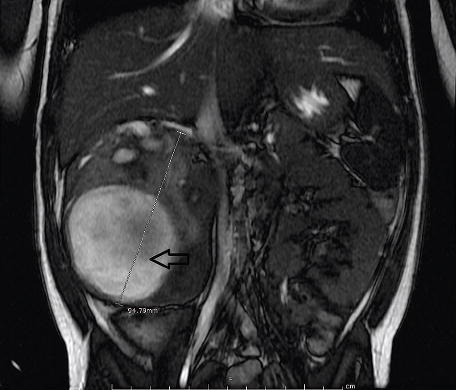
What is known so far is that 90% of the children with this disorder develop a rare pediatric kidney cancer known as Wilms tumor. Undescended testes and severe proximal hypospadias are also associated with this disorder. The Journal of the American Academy of Physician Assistants (JAAPA) recently released an article describing the case of a 3 year old patient affected by this syndrome. The authors Shawn C. Smith, Barry Chang and Laura Beth Fleming are all from the Cardon Children Medical Center in Mesa, AZ where the patient was admitted. The article describe how the authors of the article diagnosed the disorder and which treatments were used to treat the patient. The complete article can be found here
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog





 Human papillomavirus is the most common sexually transmitted infection. It is a dangerous infection because it can lead to cancer many years later. The best way to prevent developing HPV-associated cancer is to get vaccinated during preteen and early teen years. Boys and girls should get vaccinated before they start any kind of sexual activity for the vaccine to be the most effective. To be fully protected boys and girls should receive 3 doses over a year and half (one dose every six months). The New York Health department is campaigning for the vaccine as recent statistics show that on average in New York City only 40% of girls 13 to 17 years old and 22% of boys 13 to 17 years old have received the 3 doses. In Staten Island, Central/Southern Brooklyn, and Greenpoint/Williamsburg, statistics show only 5.8% to 25.1% of girls aged 13-17 and 0% to 5.9% of boys aged 13-17 received all three doses of the vaccine.
Human papillomavirus is the most common sexually transmitted infection. It is a dangerous infection because it can lead to cancer many years later. The best way to prevent developing HPV-associated cancer is to get vaccinated during preteen and early teen years. Boys and girls should get vaccinated before they start any kind of sexual activity for the vaccine to be the most effective. To be fully protected boys and girls should receive 3 doses over a year and half (one dose every six months). The New York Health department is campaigning for the vaccine as recent statistics show that on average in New York City only 40% of girls 13 to 17 years old and 22% of boys 13 to 17 years old have received the 3 doses. In Staten Island, Central/Southern Brooklyn, and Greenpoint/Williamsburg, statistics show only 5.8% to 25.1% of girls aged 13-17 and 0% to 5.9% of boys aged 13-17 received all three doses of the vaccine. Our Partner New York Medical Malpractice Attorney
Our Partner New York Medical Malpractice Attorney 
