Articles Tagged with failure to diagnose
“From Missed Diagnosis to Lifelong Harm: Lessons for Patients, Doctors, A.I., and the Law”
 In a case highlighted by The New Yorker—“If A.I. Can Diagnose Patients, What Are Doctors For? Large language models are transforming medicine—but the technology comes with side effects,” by Dhruv Khullar—we’re reminded how a missed diagnosis can spiral into life-altering harm and how patients increasingly turn to A.I. for answers when medicine falls short. The story of Matthew Williams, whose cecal volvulus was initially dismissed as “constipation,” illustrates both the stakes of diagnostic error and the complicated role A.I. now plays in modern care.
In a case highlighted by The New Yorker—“If A.I. Can Diagnose Patients, What Are Doctors For? Large language models are transforming medicine—but the technology comes with side effects,” by Dhruv Khullar—we’re reminded how a missed diagnosis can spiral into life-altering harm and how patients increasingly turn to A.I. for answers when medicine falls short. The story of Matthew Williams, whose cecal volvulus was initially dismissed as “constipation,” illustrates both the stakes of diagnostic error and the complicated role A.I. now plays in modern care.
In 2017, Matthew Williams went from an active life to one shaped by fear of everyday foods after an emergency visit that clinicians dismissed as “probable constipation.” A missed diagnosis of cecal volvulus—an intestinal twist that cuts off blood flow and requires urgent surgery—cost him roughly six feet of intestine, and with it the ability to eat freely, social comfort, and a measure of his former life. Years of follow-up care, repeated consultations, and dietary restrictions followed before a simple experiment with an A.I. tool helped point toward a dietary explanation that clinicians had not identified.
How a missed diagnosis becomes medical malpractice
Medical Negligence and the Dismissal of Patient Concerns: A Growing Patient Safety Crisis
 As medical malpractice attorneys, we know how devastating medical negligence can be — and one of the most overlooked yet dangerous forms of negligence is dismissing patient concerns. According to the ECRI Institute, this issue ranks as the #1 patient safety concern for 2025, and for good reason. When doctors ignore, downplay, or fail to investigate symptoms, they put their patients at risk for misdiagnosis, delayed treatment, and serious harm.
As medical malpractice attorneys, we know how devastating medical negligence can be — and one of the most overlooked yet dangerous forms of negligence is dismissing patient concerns. According to the ECRI Institute, this issue ranks as the #1 patient safety concern for 2025, and for good reason. When doctors ignore, downplay, or fail to investigate symptoms, they put their patients at risk for misdiagnosis, delayed treatment, and serious harm.
Unfortunately, this is not a rare occurrence. A 2023 survey found that 94% of patients reported having their symptoms ignored or dismissed by a doctor. In medical malpractice cases, we often see that this type of negligence results in worsened conditions, unnecessary suffering, and, in some cases, preventable deaths.
What Is Medical Gaslighting—and When Is It Medical Malpractice?
Webinar: A $120 Million Dollar Verdict – How did it Happen? Discussed from Start to Finish

NYSTLI Dean Anthony Pirrotti, Jr., Esq., will be hosting a Discussion with our managing partner and celebrated Trial Attorney Ben Rubinowitz, Esq.; Trial Judge Paul. I. Marx; and Defense Attorney Alfred Vigorito, Esq. next Monday May 20, 2024 from 5:00 to 7:00 PM ET.
Ben and our law firm handled a complex Stroke case involving a 41-year-old individual who was employed, married, and had children. Due to alleged malpractice, he ended up in a nursing home, unable to care for himself or his family. We will discuss the development of this malpractice case, including medical and defense aspects, discovery, depositions, and Motions in Limine. We will emphasize the significance of pleadings and expert responses for both the plaintiff and defendant and how these issues influenced the trial.
Topics include jury selection, binding statements and omissions during jury selection and openings, cross-examination of plaintiff and defendant witnesses, dismissal of a third-party defendant, the potential repercussions of aggressively attacking a witness, leveraging the defendant doctor as an expert, and the introduction of newly asserted cross-claims at trial. Additionally, we will explore the understanding of 50-A and 50-B statutes, the concept of “Loss of Chance,” the valuation of loss of consortium claims, directed verdicts against a defendant, and the strategy of defendants pointing fingers at each other.
Trial Lawyer University: A case analysis by Ben Rubinowitz about his $120 million Westchester medical malpractice verdict
Our managing partner, Trial Attorney Ben Rubinowitz going to be doing a Case Analysis hosted by Nathan Werksman on Trial Lawyers University about the $120 million medical malpractice verdict he just received in Westchester. The webinar will be on January 10, 2024 at 1:30pm.
“Lee v Westchester Medical Center” is a legal case revolving around medical malpractice and delayed treatment. The patient, a 41-year-old man, suffered a Basilar artery stroke. His wife found him unconscious at 3 am, and he was subsequently transferred to Westchester Medical Center. Initially, the stroke was misdiagnosed by resident radiologist and neurologist as an infection or dissection, delaying the correct treatment by three hours. When a more experienced radiologist later identified the stroke, a thrombectomy was performed.
The plaintiff’s claim focused on this delay, arguing that it resulted in significant brain damage and severe short-term memory issues, depriving the patient of a chance for a better recovery. The defense conceded the misdiagnosis but argued that the stroke’s severity, not the delayed treatment, caused the brain damage. They posited that the damage occurred between 10 pm and the patient’s hospital arrival, and earlier treatment wouldn’t have altered the outcome.
The Silent Epidemic of Diagnostic Errors
 Misdiagnosis of diseases and medical conditions is leading to an estimated 800,000 cases of permanent disability or death each year according to a recent study published by researchers at the Johns Hopkins Armstrong Institute Center for Diagnostic Excellence, in partnership with researchers from the Risk Management Foundation of Harvard Medical Institutions Inc.
Misdiagnosis of diseases and medical conditions is leading to an estimated 800,000 cases of permanent disability or death each year according to a recent study published by researchers at the Johns Hopkins Armstrong Institute Center for Diagnostic Excellence, in partnership with researchers from the Risk Management Foundation of Harvard Medical Institutions Inc.
Misdiagnosis is not a mere statistic; it is a human tragedy that affects hundreds of thousands of patients and their families every year. The report reveals that approximately 371,000 people lose their lives, while another 424,000 suffer from permanent disabilities annually due to misdiagnosis. These disabilities encompass brain damage, blindness, loss of limbs or organs, and even metastasized cancer. Behind these numbers are real individuals whose lives have been irreversibly altered or lost due to medical negligence.
The Top Culprits: Stroke and Other Common Diseases
Missed and delayed diagnoses, a major patient safety concern
 Missed and delayed diagnoses are common medical errors that can lead to serious injury and death. This morning the Daily Mail wrote about an 11 year old boy who died from severe bowel obstruction after a doctor misdiagnosed him with constipation and sent him back home. The doctor neglected to send him for an X-ray despite symptoms consistent with bowel obstruction.
Missed and delayed diagnoses are common medical errors that can lead to serious injury and death. This morning the Daily Mail wrote about an 11 year old boy who died from severe bowel obstruction after a doctor misdiagnosed him with constipation and sent him back home. The doctor neglected to send him for an X-ray despite symptoms consistent with bowel obstruction.In the US it is estimated that 12 million adults or 1 out of 20 patients are misdiagnosed every year
Failure to Diagnose Alcohol Withdrawal Symptoms
 Failure to diagnose alcohol withdrawal symptom (AWS) can be medical malpractice that may cause severe injury or even death in some cases. The ECRI Institute is looking at options to better “Identify Alcohol Withdrawal Symptoms Early and Ease Patients’ Care”.
Failure to diagnose alcohol withdrawal symptom (AWS) can be medical malpractice that may cause severe injury or even death in some cases. The ECRI Institute is looking at options to better “Identify Alcohol Withdrawal Symptoms Early and Ease Patients’ Care”.
An estimated 20 % of the patients that are admitted in US hospitals show symptoms of alcohol abuse or dependence. Those that are admitted for alcohol poisoning and detoxification may be difficult to treat but their alcohol withdrawal symptoms will usually be properly diagnosed and addressed.
Patients at a higher higher risk to be misdiagnosed for alcohol withdrawal symptoms are those who are admitted for a different medical condition than alcohol intoxication or dependence.
A faster and easier diagnosis of bacterial infections in newborns with fever

Fever is usually one of the first symptom of a bacterial infection. However it can also be caused by other medical conditions. When a health care provider evaluates a young infant with fever and suspect an infection, there is no quick way to find out if the infant suffers from a bacterial infection. The actual method consists in isolating live bacteria from blood, urine or spinal fluid and grow a bacteria culture in a laboratory. This may require difficult and traumatizing medical procedures such as spinal tap. Additionally the infant may necessitate hospital admission and an antibiotic prescription until the results of the tests are available.
A recent study that was published on Aug. 23, 2016 in the Journal of the American Medical Association found that through advances in genetic sequencing technology it may soon be possible for doctors to diagnose bacterial infections in infants with fevers quickly and in a non invasive manner. More work is needed but in the future only a small blood sample may be enough to immediately determine if an infant suffers or not from a bacterial infection.
How to treat and diagnose desmoids tumors?
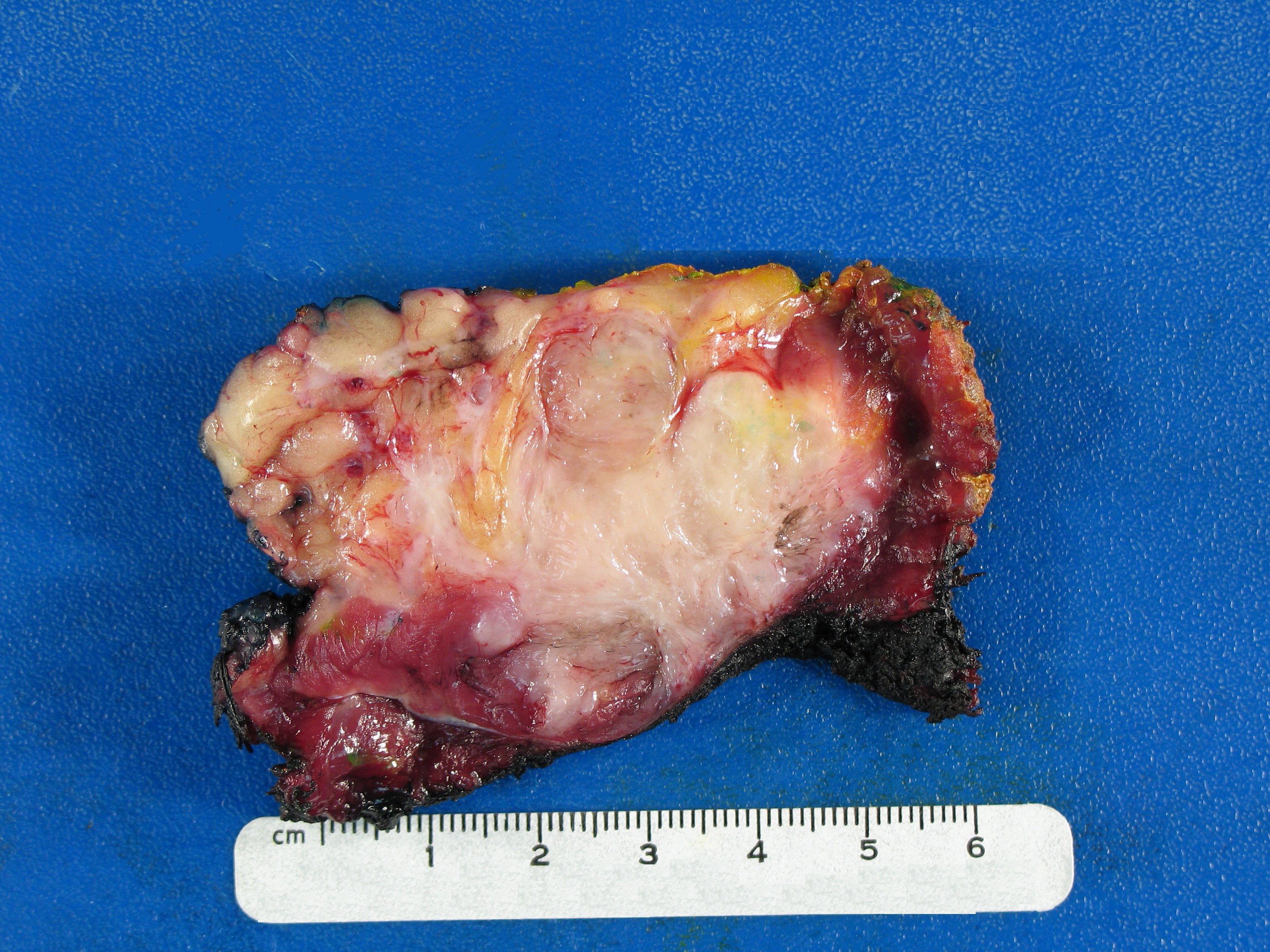 Although very rare, failure to diagnose and treat desmoids tumors, also called aggressive fibromatosis, a tumor that develops in the fibrous tissue that forms tendons and ligaments, can be medical malpractice. Desmoids tumors are very rare and difficult to diagnose and doctors are still debating what is the most appropriate categorization and treatment. In a recent article in the Washington Post, Sandra G. Boodman writes about a 24 year woman who suffered several episodes of excruciating stomach pain before being diagnosed and treated for a desmoid tumor.
Although very rare, failure to diagnose and treat desmoids tumors, also called aggressive fibromatosis, a tumor that develops in the fibrous tissue that forms tendons and ligaments, can be medical malpractice. Desmoids tumors are very rare and difficult to diagnose and doctors are still debating what is the most appropriate categorization and treatment. In a recent article in the Washington Post, Sandra G. Boodman writes about a 24 year woman who suffered several episodes of excruciating stomach pain before being diagnosed and treated for a desmoid tumor.
Johanna Dickson was 23 years old when the first symptoms of the disease occured. She had just come back from South Africa when she suffered a first episode of acute abdominal pain. She thought she caught some type of stomach bug in her last trip. The family doctor sent her to the hospital for various tests but nothing was found and the pain disappeared.
Another crisis happened six months later but it went away quickly so she didn’t even bother to see a doctor.
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog




