Most common skin cancer misdiagnoses
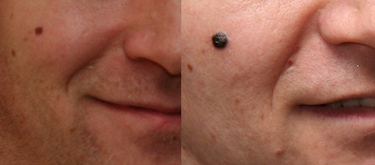 May is recognized as Skin Cancer Awareness Month. It is a crucial time to educate and inform the public about the prevalence, risk factors, and early detection of skin cancer. By increasing awareness, we aim to encourage individuals to take proactive steps to protect their skin and seek prompt medical attention when necessary. However, even with increased awareness, misdiagnoses can occur, leading to delayed or inappropriate treatment.
May is recognized as Skin Cancer Awareness Month. It is a crucial time to educate and inform the public about the prevalence, risk factors, and early detection of skin cancer. By increasing awareness, we aim to encourage individuals to take proactive steps to protect their skin and seek prompt medical attention when necessary. However, even with increased awareness, misdiagnoses can occur, leading to delayed or inappropriate treatment.
There are several types of skin cancer misdiagnosis:
- Basal Cell Carcinoma (BCC) Misdiagnosis: Basal cell carcinoma is the most common type of skin cancer. Unfortunately, it can be misdiagnosed as a benign condition such as a cyst or a harmless skin lesion. Due to the potential for misdiagnosis, patients might not receive the timely treatment they need.
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog



 Medical Malpractice may have been committed on many American Africans who were previously diagnosed with hypertrophic cardiomyopathy. A recent study found that some genetic variations that were linked to this condition were indeed harmless. These specific genetic variations were found more often in black Americans than in white Americans. Therefore many patients from African descent may have been misdiagnosed or are still being
Medical Malpractice may have been committed on many American Africans who were previously diagnosed with hypertrophic cardiomyopathy. A recent study found that some genetic variations that were linked to this condition were indeed harmless. These specific genetic variations were found more often in black Americans than in white Americans. Therefore many patients from African descent may have been misdiagnosed or are still being 

